
Everything You Need to Know About Insomnia.
Quick Links
4 THINGS TO KNOW ABOUT INSOMNIA
A few rough nights here and there are normal. Even a stretch of poor sleep for a week or two doesn’t mean something is wrong.
“Sleep hygiene” tips (avoiding caffeine, keeping your bedroom cool, etc.) don’t treat insomnia disorder.
If you struggle to fall asleep or stay asleep 3 nights a week or more for over a month — and it’s dragging down your days — you may have insomnia disorder. Talk with your healthcare provider about treatment options.
The #1 treatment for insomnia disorder is cognitive behavioural therapy for Insomnia (CBT-I).
Understanding Insomnia
“Insomnia is a natural phenomenon that is part of normal life. The issue is when it becomes a recurring problem… .”
Wait…What? Insomnia is normal?
Yes! Short-term insomnia is a completely natural human experience.
Sleep often gets shaky when life gets stressful or unpredictable. Maybe you’re starting a new job, going through a breakup, or juggling too many things at once. Sleep struggles can be a signal that your mind and body are asking for some extra care. Yet, sometimes poor sleep shows up without any clear reason at all.
Most of the time, things naturally settle back into place. Short-term insomnia can last for days or weeks. Although it can be unpleasant, this is part of life.
So how do I know when it’s more than just a rough patch?
You may have insomnia disorder (also called chronic insomnia, a treatable condition) if you notice:
1) Too much wakefulness at night






2) Daytime consequences
Having trouble falling or staying asleep? You are not alone! Insomnia is the most common sleep disorder.

In Canada right now:
9.3M people (1 in 5) are dissatisfied with their sleep
6.7M people (1 in 6) meet criteria for insomnia disorder
Keep in mind! It is perfectly normal to:
Take up to 30minutes to fall asleep
Wake up several times during the night, as long as you are able to fall back to sleep

3) Your sleep problems are not mainly explained by something else, like:
Too little time for sleep
For example, having a window of only 4 hours to sleep because or work or other commitments could make you feel pressured. You may get stressed about falling asleep quick enough or waking up on time. Not only would you be getting too little sleep, but the pressure to sleep within this limited period could make it more difficult to sleep.
A disruptive sleep environment
For example, your bed partner’s snoring or your pet moving around can make it harder for you to doze off or wakes you up at night. Also, when facing difficult life circumstances, some of us may feel unsafe in our home or our neighborhood at night.
Medications or other drugs
Your sleep can get worse after you start a new medication or even just change the dose. This is worth discussing with your healthcare provider. For instance, adjusting the dose of certain medications or even just the time at which you take them can sometimes help.
Other sleep disorders
Several other sleep disorders can look like insomnia, like periodic limb movement disorder (“kicking” at night, typically without noticing it), restless legs syndrome (discomfort in your limbs – often the legs – at rest and during the evening) or sleep apnea (breathing problems during sleep) to give a few examples. These other sleep disorders may call for other treatments than those for insomnia. As such, it is important to ensure they are not the main culprits. The identification of most of these sleep disorders require a sleep test.
Other health conditions
You may feel that your sleep issues are entirely caused by a physical or mental health condition. It’s still worth a discussion with your healthcare provider to see if some modifications to your treatment plans could be done to attenuate the impacts on your sleep. Your care provider could also suggest strategies that could attenuate the impacts on your daily life.
Keep in mind! Even if another condition affects your sleep, you may also have insomnia. Treating insomnia directly can help restore your sleep and support your overall health and well-being.

“…but is it really insomnia?”
I sleep less than 7h per night, but when I think of it… It does not seem to be impacting my days.
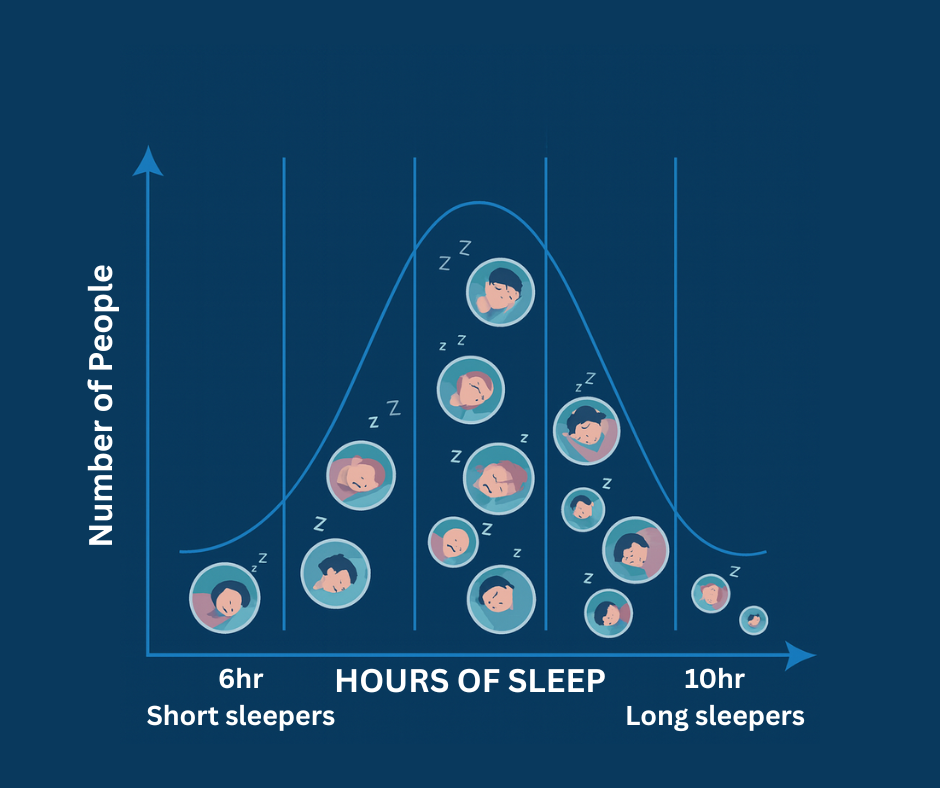
Everyone has different sleep needs. Although many people sleep 7 to 9 hours on average, some of us need more sleep and some need less.
This is in part determined by our genetic make-up. There are also normal changes in sleep as we age.
If you sleep less than most people, but wake up feeling refreshed and have no issue functioning during the day, you may just be a short sleeper. This is likely not insomnia disorder.

My insomnia seems to take a break during the week-end.
Perhaps you have no difficulty sleeping when you are free from work, family or social constraints – when you can sleep at the time that suits you best.
Have you ever thought about the timing at which it may be easier for you to fall asleep and wake up? How well does your “ideal” sleep schedule align with your actual sleep schedule?
If you are a night owl or an early bird, your prime time may be in the late evening or early morning. This may make it more difficult to fall asleep and to wake up at the time when most people do. Yet, when you are free to go to bed and wake up on your ideal schedule, you may find that sleep comes much more easily.
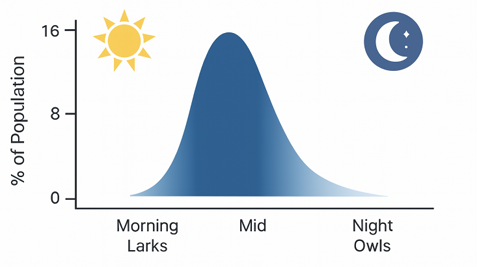
If so, there is a possibility that you do not have insomnia, but rather that your biological clock is running at an unusual time.
Specific treatments – different than what we would do for standard insomnia – can help shift your biological clock earlier or later. Keep in mind though that some people have insomnia disorder and unusual biological clock timing at the same time.
In doubt? Talk about it with your healthcare provider!
Causes of insomnia disorder and how it develops
What causes insomnia disorder?
Insomnia can be a symptom (that is, trouble falling asleep or staying asleep) OR it can be a disorder (when there are daytime complaints and the insomnia becomes frequent and chronic).
In the weeks in which insomnia starts to become more regular, something we call “hyperarousal” occurs. Think of hyperarousal like a car whose engine idles higher —it keeps running even when you’re trying to rest. This heightened state makes you feel less sleepy, which can help you function during the day, but it also makes it much harder to fall or stay asleep at night. People with insomnia often describe this feeling as being “tired but wired.”

As the weeks go by, you may have a new tendency to spend more time awake in bed then you used to in attempt to get more sleep. The bed then becomes the place where you are awake, rather than the place where you sleep. As people cope with insomnia symptoms, they are more likely to:
Spend more time in bed, for example, going to bed early, napping, sleeping in

Bottom line: What first triggered insomnia—whether age, illness, stress, or something less obvious—often matters less than how we respond to it. People tend to cope with insomnia in similar ways, and these coping behaviors can unintentionally disrupt the body’s natural sleep systems. All chronic insomnias are maintained by the same things:
“Try” to sleep, for example, playing white noise, using black out blinds, using diet supplements, alcohol, etc. These coping strategies can have the unintended effect of interfering with the systems that control sleep. These sleep systems require regularity and activity.

The coping attempts described above also have one thing in common: an attempt to “try to make” sleep happen. Many people lose faith in their sleep system and try harder to fix it with substances, medications, gadgets or trying to control their environment. This rarely works because sleep is not a matter of trying, but of letting go.
The hyperarousal that appears when the insomnia becomes chronic
The repeated pairing of the bed with sleeplessness — so that getting into the bed makes you feel immediately alert
Less activity, less regularity and/or more time in bed — all behaviors that interfere with your sleep system. Trying to sleep — instead of trusting your sleep system




This is good news because it means you can fix it by learning about your sleep systems and how to get them to work for you, along with some tricks to reverse hyperarousal and the association of your bed as “the place you are awake.”

It’s a sleep disorder, but it feels like if affects me all the time!
Exactly. Even though insomnia arises from nighttime issues, its fingerprints are all over the daytime too.
If you have insomnia disorder, you feel clear impacts of this lack of sleep during the day. For instance, you may be exhausted, yet unable to nap. You may feel like you have no energy and that everything requires more effort. Your thinking skills may become less reliable, with a foggy mind, poor concentration, and memory problems. Your mood may switch to the low side and perhaps you become more irritable than usual. This can put a strain on your relationships, your performance at work or at school, and your overall quality of life.
This is the focus of a treatment called Cognitive Behavioral Therapy (CBT)

Become less active and regular in their activities


Having insomnia doesn’t mean every night is sleepless. In any given week, you probably have some bad nights and some better nights.
This unpredictability is tough. Not knowing if you’ll get rest — especially before a big day — can create a ton of stress at bedtime. The more you worry about sleep, the harder sleep tends to come.
Yet, the reality is that the dynamics of insomnia are often unpredictable.
It is common to worry that your insomnia may be different or not treatable. It is common to worry that insomnia can’t be treated, especially if you’ve been living with it for a long time. Sadly, it is not rare for people to suffer from insomnia for 10 years before receiving effective treatment.
I thought I beat it, but now it’s back again!
Insomnia tends to come and go. Sometimes you’ll have weeks or months of decent sleep, only to see the old pattern return. This is very common.
Don’t jump to conclusions too quickly though! This may be just a bout of normal short-term insomnia. Only time can tell if you are on your way to another episode of chronic insomnia.
Even if you are, it doesn’t mean you have to be back to square one when this happens. Once you learn effective tools to manage insomnia, you’ll be much better equipped to calm future flare-ups before they take over.

Another reason for worrying your insomnia is not treatable can occur when you have another condition along with your insomnia, including medical disorders, like cancer, or mental health challenges like anxiety or depression. You may also think that insomnia is inevitable because you are getting older or going through menopause. Whether someone has insomnia disorder only or another condition on top of insomnia disorder, the insomnia symptoms are the same, and the insomnia treatment is the same.
Keep in mind! Because some of the daytime effects of insomnia disorder are the same as they are in some of these other conditions (e.g., fatigue, concentration problems and mood disruptions), many people, including health providers, can mistakenly think it is not insomnia disorder.
If you have had sleep issues for more than 1 month, the fact that you also have another condition does not change that you have an insomnia that warrants treatment.

Insomnia is not your fault. Your body and brain are not ‘broken.’ They just need some retraining.
Insomnia disorder is a 24h condition:
It affects not just your nights, but also your days
All in all, insomnia disorder is not just about losing sleep. It’s about how much sleep loss changes the way you live your life.
Why does my sleep feel so unpredictable?
When left untreated, insomnia disorder often sticks around, sometimes for years. With the right help, you don’t have to just “live with it.”
Is my insomnia different?
Getting help for insomnia
I think I may have insomnia… What should I do?
Unlike some other sleep disorders, insomnia doesn’t usually require fancy machines or overnight sleep tests for diagnosis. The diagnosis of insomnia disorder is based on a subjective dissatisfaction with sleep. As such, to see if you have insomnia or not, your healthcare provider may simply ask you some questions about your sleep patterns, health history, medications.
You can start by answering a few questions using our screener for insomnia disorder.



You can print your results and share it with your healthcare provider for further assessment and treatment.


You are the best judge! Insomnia is diagnosed based on your experience and how it impacts you.

Sleep hygiene and medications are NOT the recommended first line treatment for insomnia disorder. If you have insomnia disorder, the first option you should be offered is cognitive behavioral therapy for insomnia (CBT-I).
Ask your doctor to get a referral for a professional specialized in CBT-I (often times this is a psychologist). You may also be able to access CBT-I for free through some research studies


Keep in mind! A sleep test (like a polysomnogram) is typically not needed to determine if you have insomnia. However, if your sleep is not refreshing or if you have daytime sleepiness that’s hard to resist, your healthcare provider could suspect that another sleep disorder aside from – or in addition to - insomnia could be at play. If so, they may recommend a sleep test to be sure to direct you towards the best treatment(s).
They may also order some blood tests to screen for medical conditions that can affect sleep, like thyroid problems for example.

Tips to help you plan your insomnia discussion with your healthcare provider
Be ready to share:

You might want to ask them:
Could another condition or medication be affecting my sleep?
What treatment options are available to me?
Could cognitive-behavioral therapy for insomnia (CBT-I) be right for me?
What are the possible pros and cons of sleep medications?
How long should I try a treatment before deciding if it works?
What community supports are out there?
When should we schedule a follow up appointment?
What should I do if my sleep gets worse?
*Be ready to ask if CBT-I is right for you! (some healthcare providers do not know about CBT-I)
What your typical sleep looks like
Bed and wake-up times (including differences between weekends vs weekdays)
How long it takes you to fall asleep
How often do you wake up during the night and for how long
What does a ”bad night” look like and how often does it happen
How long you’ve had these issues
Any changes in your medications (prescribed and non-prescribed) around the time when your sleep issues started
Any physical or mental health concerns that may affect sleep
How your sleep issues affect your day-to-day life
If you want to involve a relative in your care plan
*You can bring in your results from the screener
What treatment options are available to me?
If you are having trouble sleeping, your healthcare provider should talk with you about your sleep and how it is affecting your daily life. They should ask you about your sleep and medical history. If you have another condition along with chronic insomnia, this should not delay treatment for the insomnia disorder. If you have insomnia disorder, you should be offered cognitive behavioral therapy for insomnia (called CBT-I) as a first-line treatment.

CBT-I is very brief (4-6 sessions), but most people remain well for years afterwards, so it is preferable to sleep medications that do not remain effective and can cause side effects, particularly in the elderly.
People with insomnia disorder should not be offered sleep medications until they have tried CBT-I. If they receive medication, it should be:
An effective medication
At the lowest possible dose
For the shortest possible duration (i.e., typically 2 weeks)
Only after a discussion about the risks associated with the prescribed medication
Why use a “therapy” for insomnia disorder?
CBT-I is recommended over medication because it is at least as effective, but safer, and it lasts for years after completing it. CBT-I is based on research telling us what keeps chronic insomnia around, even if what initially caused the insomnia is resolved.




The “C” in CBT-I are “cognitions” or thoughts. CBT-I focuses on how the way we think about sleep can actually can become a problem on its own and make sleep worse. For example, worrying about not sleeping or about how tired you’ll feel the next day can increase anxiety, which in turn makes it even harder to sleep. Learning strategies to deal with these thoughts can reduce worry and help rebuild confidence in your body’s natural sleep system.
The “B” in CBT-I stands for behaviors. CBT-I uses behaviors to reset our body’s internal clock and to increase sleepiness, so that we are better able to sleep. Developing a tailored schedule and set of rules to increase the likelihood of sleeping while in bed, can get rid of the insomnia disorder for good.
The “T” in CBT-I stands for therapy! Unlike medications that target arousal only, CBT-I gives you a toolbox to address all of the key causes of chronic insomnia and leverage your body clock and sleep drive systems.
The “I” in CBT-I stands for insomnia!
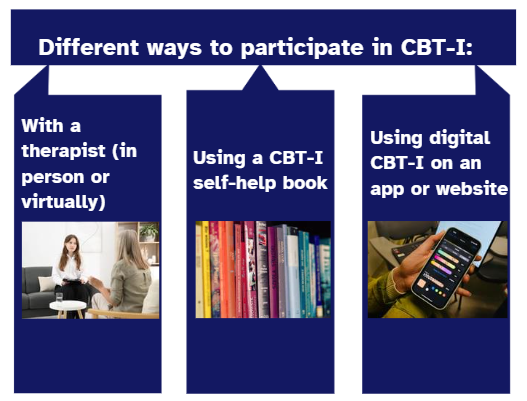
Where can I get CBT-I?
In Canada, there is a growing province-by-province directory in which you can contact people who provide this treatment either in person, via telephone or virtually on the computer. Unless your family doctor can give you a referral, you will typically pay for this. You can ask your provider if they have a “sliding scale” (discounted rate based on lower income) and how many sessions they will provide. If you are focusing on CBT-I only, you can typically expect 4-6 sessions.

Provider Directory for Cognitive behavioural therapy for Insomnia (CBT-I)
Since CBT-I is often offered by trained psychologists, you can also contact your province's psychologists college.
Click HERE to access the list of Provincial and Territorial regulatory bodies.
Free resources for CBT-I
Books
Evidence-based digital self-help tools and websites
Research studies
You may also be able to receive CBT-I for free as part of a research study. Click HERE to access current studies.
Your Questions, Answered
-
The number one theory of people with insomnia is that their insomnia is caused by a “noisy mind.” Interestingly, there are techniques often used as part of CBT-I that can decrease noisy minds but in every study, this does not lead to any improvement in sleep. In contrast, some of the techniques of CBT-I that help you to fall asleep faster and stay asleep longer are as effective in quieting the mind. It turns out that the noisy minds people experience is a RESULT of the insomnia, not the CAUSE of it. CBT-I will help with sleeping and noisy minds.
-
Yes! The original tests of CBT-I were with middle-aged and older adults, so we know they are highly effective in this age range.
-
We use something different with kids [link to pediatrics]. Child treatments typically focus on parents strictly controlling bedtimes and wake times, but adolescence is a time when teens are supposed to be learning to be more independent.
Teens face unique sleep problems that limit their ability to use child sleep resources.
Teens can benefit from CBT-I . However, many teens do not suffer from insomnia only; they can also experience daytime sleepiness and excessive sleeping on the weekend. This situation is caused by their body clock being out of sync with early school start times during the week. A treatment called Transdiagnostic Circadian Youth treatment combines CBT-I with other sleep strategies to solve the unique challenges of teen sleep problems. There is a free Canadian app on the App Store and Google Play called Doze: goodnight mind for teens.
-
You can talk to any prescriber about medication for insomnia. Many people use over the counter sleep medications or sedating medications, but these do not have good scientific evidence and often have serious side effects. Diet supplements also do not have good evidence and there are concerns that some may have side effects or drive bad reactions with other medications.
-
A sleep diary is a tool to document your sleep patterns over 1-2 weeks. In this diary, you would note down the times at which you go to bed and wake up, how often you wake up during the night and or how long, the time you spend napping during the day, as well as other things that may influence your sleep. This is a helpful first step to understand your sleep issues.
Click here to start filling out a sleep diary


